May 18, 2026

Header top telephone number
- Clinic Appts218-927-2157
- Hospital218-927-2121
- Sign in toMyChart
- Online Scheduling
- Apply now!Careers

Header top telephone number
- Clinic Appts218-927-2157
- Hospital218-927-2121
- Sign in toMyChart
- Online Scheduling
- Apply now!Careers
UROLOGY
urology care in aitkin, mn - advanced, compassionate treatment close to home
Whether you’re managing a chronic urologic condition or seeking relief from new symptoms, Riverwood offers a full spectrum of services—from minimally invasive therapies to robotic-assisted surgery—right here at home.
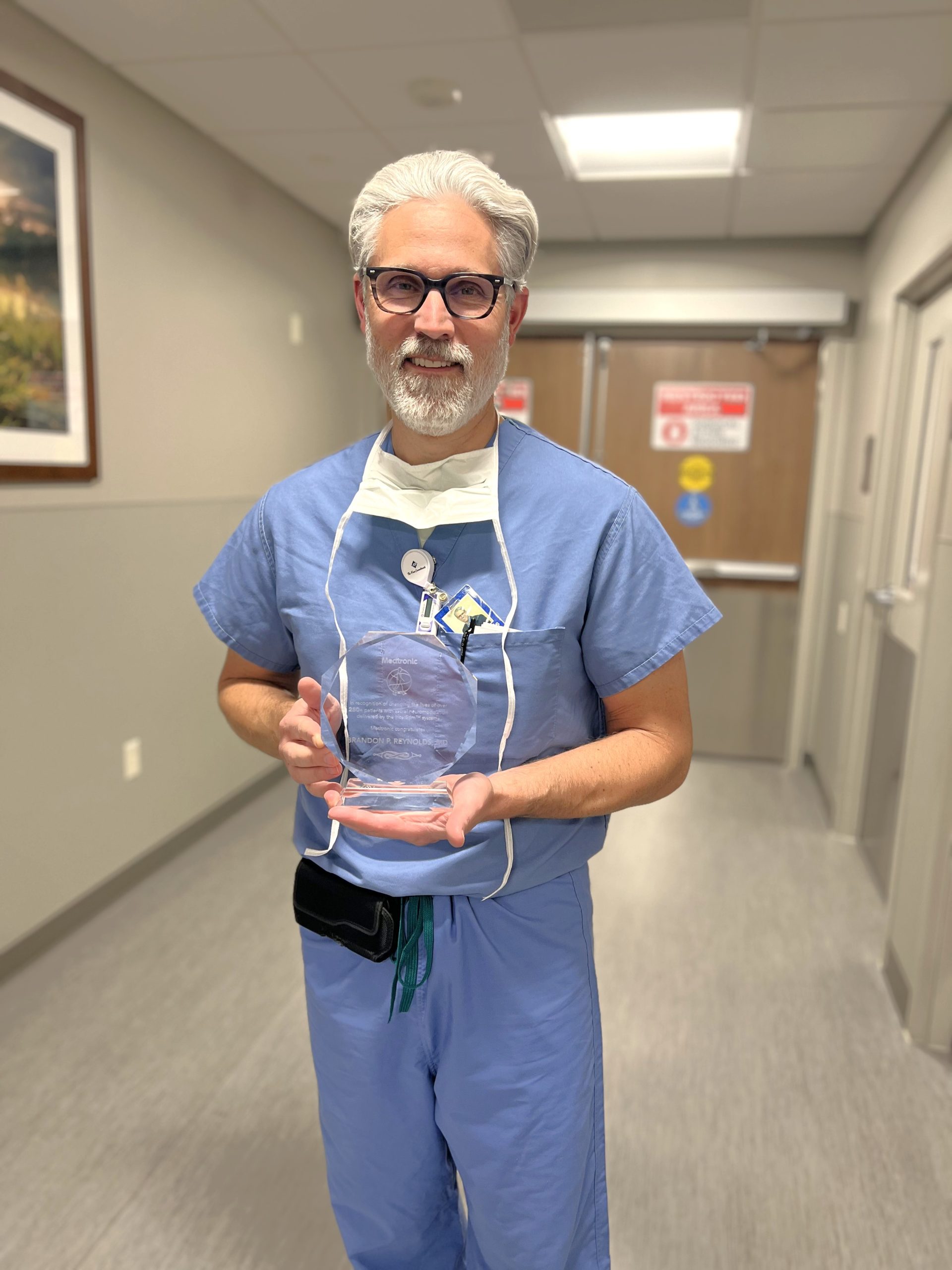
Center of Excellence Physician
Practicing at Riverwood since 2020, Dr. Brandon Reynolds, MD, has been designated as a Medtronic InterStim™ Center of Excellence physician. InterStim™ is a minimally invasive procedure for treating overactive bladder, urge incontinence, and fecal incontinence. Riverwood is one of three practices in the state of Minnesota that are designated Center of Excellence for InterStim™.
In July 2024, Dr. Reynolds was designated as a UroLift™ System Center of Excellence physician. Dr. Reynolds is the only urologist north of the Twin Cities to earn this unique UroLift achievement. This designation is awarded to physicians who have attained advanced training with the UroLift™ System, which offers rapid relief for benign prostatic hyperplasia (BPH) symptoms, commonly causing men to experience frequent and urgent urination.
Additionally, Dr. Reynolds has been recognized as a GreenLight™ Center of Excellence physician. This distinction highlights his expertise in performing GreenLight™ laser therapy, a minimally invasive treatment for BPH that provides long-lasting relief from urinary symptoms with faster recovery times compared to traditional surgical methods



Select the videos below to hear from Brandon Reynolds, MD, about our urology services.
Urology Videos

3:11

2:13

1:51

3:34

2:01
our urology services
1. Urgency: A sudden and overwhelming need to urinate immediately.
2. Frequency: Urinating more than 8 times a day (normal is about 4-6 times daily or every 3-5 hours)
3. Urge incontinence: Urine leakage (wetting accident) that follows a sudden urge (amount can be anywhere from a few drops to the entire contents of bladder)
4. Nocturia: Waking up 2 or more times during the night to urinate (most people can sleep 6-8 hours without having to urinate)
Overactive bladder is not a normal condition at any age. Without treatment, symptoms may go from merely bothersome to becoming a severe urinary bladder condition. When uncontrollable urgency, frequency or leakage become a troublesome pattern, it’s time to talk to your healthcare provider about this issue.
The Altaviva™ implant is your convenient and hopeful next step, with automatic therapy delivery that can integrate seamlessly into your life – designed to keep you moving forward, wherever your journey leads. Unlike medications or injections that target bladder muscles, the Altaviva™ implant for urge urinary incontinence (UUI) targets the tibial nerve that helps control normal bladder function.
Overactive Bladder
Bladder control problems affect tens of millions of people every day. If you’re one of them, you should speak up.
Does this sound familiar?
Urinating more than 8 times a day
Avoiding social events
Using pads to control leaks
OAB Facts
OAB is extremely common.
1 in 6 adults has OAB, or 43 million adults in the U.S.
4.5 out of 10 adults don’t seek help for overactive bladder
You Are Not Alone – Find Relief for Bladder Control Problems
Overactive bladder (OAB) is a treatable condition. It’s not a normal part of aging. And you shouldn’t have to deal with it on your own.
Medtronic Bladder Control Therapy Delivered by The InterStimTM Systems
Evidence suggests that breakdowns in the bladder-brain communication pathway may be a root cause of OAB and non-obstructive urinary retention.1,2,3 That’s why conventional treatments may not produce the results you want – they don’t directly target this miscommunication. Unlike conventional treatments, the Medtronic InterStim systems gently stimulate the sacral nerves in the pelvic area that control the bladder.4,5 This may help restore* bladder-brain communication and reduce symptoms.
Get more control with the InterStim Systems6,7
84% satisfaction among those who use it8
3X greater improvements in OAB quality of life9
82% of people achieved success† at 5 years6
Only therapy that lets you see if it works before you and your doctor decide
More than 375,000 people worldwide have chosen the Medtronic InterStim systems for more control and long-lasting relief6,7
Recharge-free and rechargeable options let you choose the right device for your lifestyle
In addition to risks related to surgery, complications can include pain at the implant sites, new pain, infection, lead (thin wire) movement/migration, device problems, undesirable changes in urinary or bowel function, and uncomfortable stimulation (sometimes described as a jolting or shocking feeling). Talk with your doctor about ways to minimize these risks.
Is InterStim Right for You?
You may be a good candidate for Medtronic Bladder Control Therapy delivered by the InterStim systems if:
You have significant OAB symptoms or non-obstructive urinary retention
You’ve tried lifestyle changes and oral medications
These therapies haven’t given you the relief you want.
Say yes to the test
Take back control with an evaluation for an InterStim system
Unlike other bladder control treatments, this therapy lets you try it first with an evaluation – like a test run, not a long-term commitment.
Here’s how it works:
The simple test starts at your doctor’s office or an outpatient center.
A lead (thin wire) is inserted in the upper part of your buttock. The lead attaches to a small external device worn discreetly under your clothes.
Stop, start, or adjust the therapy settings, with an easy-to-use programmer that resembles a smartphone.
Go about most of your regular activities for 3 to 14 days.
Track your symptoms to see if they improve
Get more personalized treatment options
After your test, talk to your doctor about the results. Together, you can choose a powerful and personalized solution for your long-term care. Your evaluation device can be replaced with an implantable device called a neurostimulator during a short, outpatient procedure.
Bladder control therapy has risks similar to any surgical procedure. The most common adverse events experienced during clinical studies include pain at implant sites, new pain, lead migration, infection, technical or device problems, adverse change in bowel or voiding function, and undesirable stimulation or sensations. Any of these may require additional surgery or cause return of symptoms. Discuss these potential risks and benefits with your doctor.
More control starts with our smart programmer
The smart programmer allows you and your healthcare provider to manage your therapy as needed. Unlike previous iterations of our technology that resembled a key fob without a display screen, our Smart Programmer allows you:
Visibility to check your stimulation level on a clear, easy-to-read screen
Adjust your stimulation with confidence that its been changed to the setting you intended
Turn stimulation on or off
Change therapy programs (as directed by your healthcare provider)
Activate MRI mode and check MRI eligibility (see more information below)
MRI Confidence
Medtronic’s proprietary SureScan™ MRI technology is what enables patients to get full-body‡ 1.5 and 3T MRI scans. It is the only sacral neuromodulation system with this SureScan technology. This means:
Full-body‡ 1.5 and 3T MRI scans
No impedance checks required prior to MRI scans
Scans allowed even if you have had out-of-range impedances
MRI mode is easy to activate or deactivate on Medtronic’s smart programmer without clinician or Medtronic interaction
Digital display for clear confirmation of MRI mode activation.
Access the Medtronic InterStim MRI Brochure to learn about our MRI Center of Excellence and MRI testing lab and for information on how to activate MRI mode on your smart programmer.
*Restored function defined as a 50% or greater reduction in dysfunctional voiding symptoms from baseline
Frequently Asked Questions
Why is this therapy different?
You can try it before you decide, and it’s reversible if you change your mind later. And unlike injections, it doesn’t require self-catheterization or repeated treatment visits.
What can this therapy do for me?
It may significantly reduce symptoms in people who have frequent urges to urinate or related frequent leaks or are unable to fully empty their bladder.1
Will it cure my condition?
No. It can be effective, but it’s not a cure. If the neurostimulator is turned off or removed, symptoms can return.
What does the stimulation feel like?
Most people describe the stimulation sensation as a tingling, flutter, or vibration in the pelvic area. It should not be painful. Stimulation settings can be adjusted, and sensations will vary from person to person.
Can I have an MRI?
People with an InterStim™ system can have a full-body‡ MRI scan under certain conditions. Your doctor will determine whether you meet those conditions.
Will insurance cover the costs?
Medicare and many private insurance companies cover this therapy. Talk to your doctor to learn more about your insurance coverage.
What is BPH?
Benign Prostatic Hyperplasia, or BPH, is a common condition in which the prostate enlarges as men get older. While BPH is a benign condition and
unrelated to prostate cancer, it can greatly affect a man’s quality of life. As the prostate enlarges, it presses on and blocks the urethra, causing bothersome urinary symptoms. If left untreated, BPH can lead to permanent bladder damage.
Symptoms include:
Frequent need to urinate both day and night
Weak or slow urinary stream
A sense that you cannot completely empty your bladder
Difficulty or delay in starting urination
Urgent feeling of needing to urinate
A urinary stream that stops and starts
If you suffer from the above symptoms, you are not alone. BPH is the leading reason men visit a urologist.
You can measure your BPH symptoms by taking the International Prostate Symptom Score (IPSS) questionnaire.
What is the UroLift System?
The UroLift® System is a minimally invasive, safe and effective procedure to treat an enlarged prostate providing rapid symptom relief and recovery of BPH symptoms. It is a proven
option for patients looking for an alternative to medications or major surgery. The UroLift® System is the only leading BPH procedure shown to not cause new and lasting sexual dysfunction.
How Does The UroLift® System Work?
The UroLift® System uses a revolutionary approach to treating BPH that lifts and holds the enlarged prostate tissue so it no longer blocks the urethra. It is the only available BPH treatment performed by a urologist that does not require heating, cutting, or removal of the prostate tissue. The procedure is typically performed using local anesthesia in a the physician’s office or ambulatory surgery center. Patients typically return home the same day without a catheter.
Frequently Asked Questions
Who is a good candidate for the UroLift® System treatment? You may be a good candidate if you are a male, 45 years of age or older, and have symptoms relating to BPH. Speak with your urologist to see if the UroLift® System treatment is right for you. If you have a known allergy to nickel, titanium or stainless steel, talk to your doctor about your allergy before getting a UroLift System treatment.
What should I expect during the treatment? Is it painful? How long does it take? If you and your doctor decide that the UroLift® System treatment is right for you, your doctor will provide you with more detailed information relating to the treatment. In general, the UroLift System is a minimally invasive treatment that entails minimal downtime. Your doctor will use the UroLift Delivery Device to deploy permanent implants to relieve obstruction caused by the enlarged prostate that is pressing on your urethra. The procedure, which usually takes about an hour, may be performed under local or general anesthesia and you may be given medication to feel comfortable during the treatment. This typically helps minimize discomfort during the procedure, though everyone’s definition for pain and discomfort varies greatly. Typically, no catheter and no overnight stay is required post-treatment.
What happens post-treatment, during the recovery period? Are meds required? After the treatment, patients typically go home the same day without a catheter. There is minimal downtime posttreatment and many patients experience symptom relief in as early as 2 weeks. Patients may experience some urinary discomfort during the recovery period. Most common side effects are mild to moderate and include pain or burning with urination, blood in the urine, pelvic pain, urgent need to urinate and/or the inability to control the urge. Most symptoms resolved within two to four weeks after the procedure.
Does the treatment affect my sexual function? Clinical studies have shown the UroLift® System treatment does not cause new, sustained instances of erectile or ejaculatory dysfunction. The same cannot always be said of other BPH therapies such as TURP, laser, and even medication.
Does my insurance cover the treatment? The UroLift® System treatment is covered by Medicare and all major private insurers. Contact your insurance provider for your specific coverage information.
An enlarged prostate can mean frequent trips to the bathroom and interrupted sleep, causing quality of life to be less than optimal. Turn to Riverwood Healthcare Center’s expert urologist for the latest and most innovative treatment options for benign prostatic hyperplasia (BPH), helping you get back to a higher quality of life. Advanced treatment options include GreenLight™ Laser Therapy.
Benign Prostatic Hyperplasia (BPH)
In men with BPH, the prostate gland is not cancerous but has become enlarged. An enlarged prostate can result in a variety of urinary tract symptoms, including frequent urination, difficulty starting or maintaining urine flow, inability to urinate, or loss of bladder control. BPH becomes more common with age, affecting more than 40 percent of men over 60, and symptoms may worsen over time if left untreated.
While many cases of BPH can be managed with medication, some patients require procedural treatment to relieve obstruction and prevent complications such as urinary retention and recurrent urinary tract infections.
GreenLight™ Laser Therapy
GreenLight™ Laser Therapy is an advanced, minimally invasive treatment option that provides rapid relief of symptoms caused by BPH. In many cases, GreenLight therapy offers a shorter hospital stay, reduced catheterization time, less bleeding, and faster recovery compared to traditional surgical approaches.
Who This Treatment Is For
GreenLight is suitable for most patients with an enlarged prostate. One of the primary benefits of GreenLight therapy is how quickly it works—most patients return home just a few hours after the procedure and are able to resume normal, non‑strenuous activities within days.
How It Works
During the procedure, the urologist uses laser energy to precisely heat and vaporize excess prostate tissue. Removing this tissue creates a larger channel for urine to pass through, rapidly restoring natural urine flow in most patients.
The Procedure
GreenLight Laser Therapy is typically performed on an outpatient or inpatient basis under general anesthesia. Many patients experience significant symptom improvement and better urine flow shortly after treatment. Your urologist can provide individualized guidance on whether this procedure is right for you and what to expect before and after treatment.
Not necessarily, although urinary incontinence occurs about twice as often in females than males. Pregnancy, childbirth, menopause and female anatomy account for the difference. But of the approximately 12 million sufferers in the United States, about one-third are men. Male incontinence is often associated with prostate problems or treatments.
Generally, it’s a good idea to call your doctor or schedule an appointment if you have a sudden onset of incontinence, if you’re having enough accidents that you need to either wear a pad for urine absorption, or if incontinence is interfering with your lifestyle.
A change in the normal balance of water salts, mineral and other components in urine creates a process known as urolithiasis in which solid mineral particles cluster in the kidneys. There are different types of stones, including calcium oxalate, uric acid, ammonic magnesium and cystine.
Certain groups of people are more prone to kidney stones, and some medical conditions can be contributors. Men in their 30s, 40s and 50s are mostly likely to get stones, and postmenopausal women and women who have had their ovaries removed are at a higher risk than normal. Other contributors include frequent urinary tract infections, insulin resistance, cystic fibrosis, gout, inflammatory bowel disease, gastric bypass surgery, hyperparathyroidism, high blood pressure, and bladder problems resulting from spinal injuries.
Drink lots of water. The most common cause of stones is an insufficient daily water intake. The goal should be to drink enough to keep your urine clear – about eight to ten glasses per day. In addition, studies have indicated that staying physically fit and keeping your weight in check can help as well.
The no-scalpel incision vasectomy has become very popular in the U.S. because of the decreased discomfort that men experience with this particular technique. We perform the no-scalpel incision vasectomy and would be happy to provide you with more information about this procedure.
The American Cancer Society recommends annual screening for all men over the age of 50, including a digital rectal exam and a PSA (prostate-specific antigen) blood test. Men with a family history of prostate cancer should start annual screenings between age 40 and 45.
One reason that screening for prostate cancer is so important as a man ages is that localized and curable prostate cancer has no symptoms. A decrease in the force of the urinary stream or other voiding issues is most likely due to benign prostatic hyperplasia (BPH) than prostate cancer. For men with localized prostate cancer and some urination problems, the explanation is that BPH is occurring coincidentally with the prostate cancer. Men with advanced prostate cancer, however, may have similar symptoms as men with BPH, including blood in the urine, painful urination, and a decreased urinary flow. Fortunately, with today’s emphasis on screening and early detection, more than nine in 10 prostate cancers are found in potentially curable stages.
Meet dr. brandon reynolds - board certified urologist and team
Dr. Reynolds and team provides the full spectrum of urologic care for men and women, specializing in medical and surgical management of:
- Kidney stones
- Incontinence
- Prostate enlargement
- Overactive bladder
- Urologic cancers
- Male genital concerns
- No‑scalpel vasectomy procedures
Rachel Bridgeford, RN, Urology Coordinator
Take a video tour of our state-of-the-art surgery expansion.
UROLOGY BLOG


October 15, 2025

September 19, 2024

August 27, 2024

August 31, 2023


September 15, 2022
Real patients. Real stories.
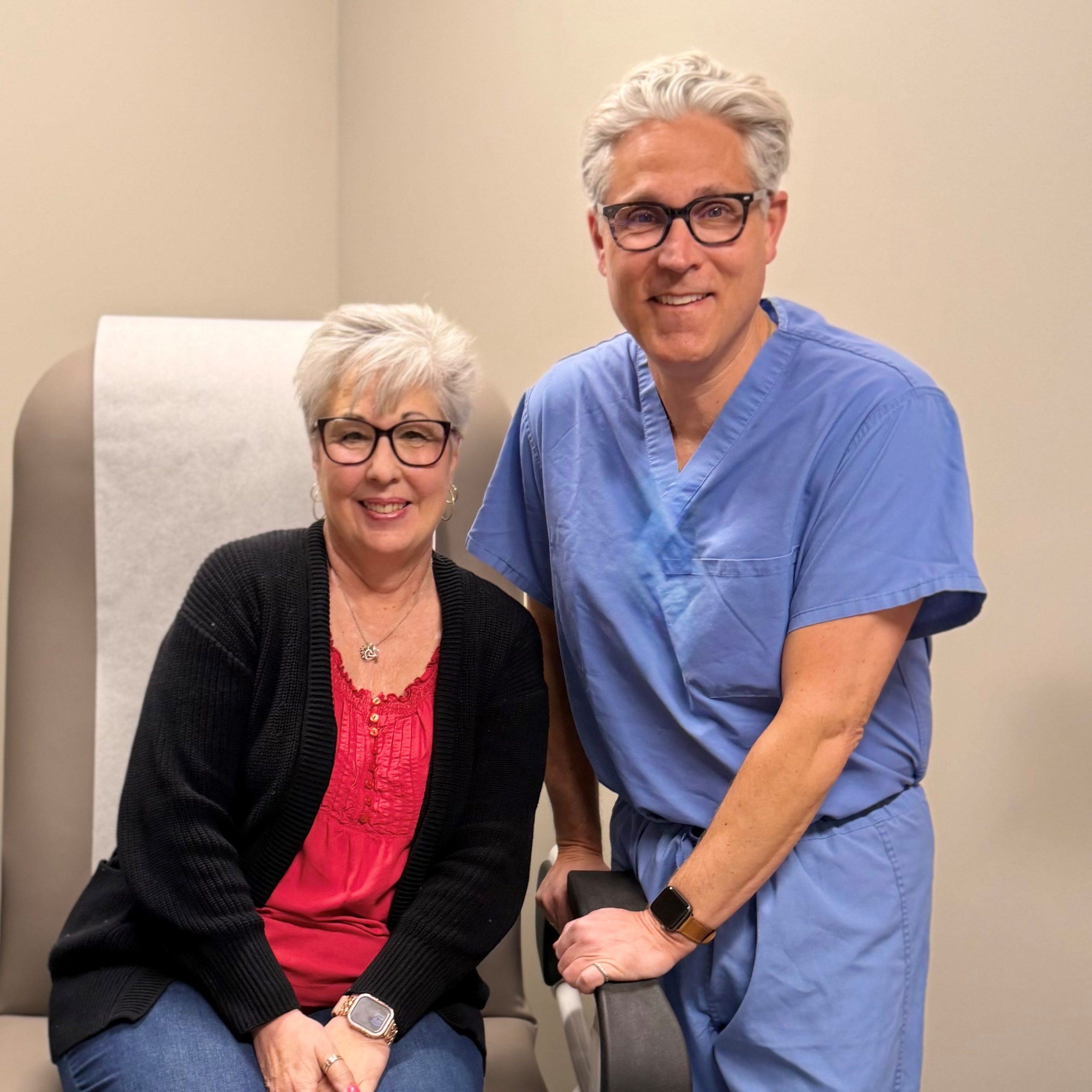
“Dr. Brandon Reynolds is a remarkable urology provider, and Riverwood is lucky to have his expertise, care, and compassion here in our community. For my first appointment, Dr. Reynolds met with me for an extended period, treated me with dignity and offered me treatments and hope for a condition that has no cure or easy solution. Amanda, the urology nurse coordinator, has also been instrumental in my care, and I appreciate her knowledge and grace during procedures. The sense of comfort I feel about the care that I receive here at Riverwood and from the whole Urology team is truly amazing.” -Alison, Patient
“Dr. Reynolds performed the UroLift procedure to relieve my symptoms, and it was a relatively quick recovery. My urinary symptoms resolved within a few days. By the end of the first week following surgery, I was back to normal, and I’ve had no problems since then. After getting up several times during the night to urinate for many years, it was so good to sleep through the night again. Dr. Reynolds was very easy to talk to and informative about how the procedure would work. The whole Riverwood team impressed me, especially the surgery nurses. When my wife and I also had colonoscopy screenings, we had a good experience as well. Everybody we met at the clinic and hospital was super helpful and nice.” - Jeffrey N
"Gary's case was challenging with a very aggressive cancer needing surgical treatment," his wife, Loretta, explains. "On the day of the surgery, Dr. Brandon Reynolds spoke to us in plain language and laid out what would happen during and after surgery. He has an excellent bedside manner, and we would trust him caring for anyone." - Gary, Grand Rapids patient
Living in a smaller rural community sometimes means having to travel out of area for excellent specialty care. In Gary’s case, the 50 miles from Grand Rapids to Aitkin was very well worth it. Unable to access a urologist who could perform surgery in Grand Rapids, Gary was referred to Riverwood Healthcare Center’s urology department when he needed treatment for prostate cancer. “Gary’s case was challenging with a very aggressive cancer needing surgical treatment,” his wife, Loretta explains. “On the day of the surgery, Dr. Brandon Reynolds spoke to us in plain language and laid out what would happen during and after surgery. He has an excellent bedside manner, and we would trust him caring for anyone. “We would also like to thank Physician Assistant Elizabeth Lilley for her role in Gary’s care, plus Amanda Peka, urology RN coordinator, who took initiative to make calls to get Gary’s surgery scheduled at the earliest available time.” Gary’s care included an overnight hospital stay, where he encountered more wonderful caring Riverwood staff, including a post-op visit from Nurse Anesthetist Lincoln Roth. Loretta adds, “Gary’s surgery was on my birthday and the successful outcome was the best present ever! “Cancer is a scary condition, and all the Riverwood staff members, from check-in through surgery and hospital nurses, genuinely care for patients with such kindness. They love their jobs, and it shows! “We would highly recommend Riverwood to anyone based on our wonderful experience.”
